This course appeared as the CPE Monthly in the December 2015 issue of Today's Dietitian. For a printable PDF of this course and exam, click here.
Despite more attention and focus on obesity as a national and global pandemic from the scientific, health care, and political communities, high rates continue to prevail. Nearly 35% of the US adult population is obese,1 and, according to the World Health Organization (WHO), deaths linked to obesity have surpassed deaths caused by being underweight.2 According to the systematic Global Burden of Disease Study 2010, deaths attributable to malnutrition, infectious disease, and maternal-child diseases are on the decline compared to 20 years ago and are surpassed by noncommunicable diseases of obesity such as heart disease and cancer.3 Beyond mortality alone, obesity is irrefutably responsible for increasing the risk of developing some of the leading causes of preventable chronic conditions. For example, obesity has been widely discussed for its role in diseases of the cardiovascular system such as heart disease and stroke; the endocrine system, such as diabetes; and the digestive system, such as fatty liver or gallbladder disease. But while those diseases get the lion’s share of media and research attention, other diseases have been associated with obesity.
This continuing education course discusses those conditions uniquely influenced by obesity to elucidate the devastating reach of this disease beyond that which is commonly discussed. The etiology of obesity will be discussed within the context of its central role in obesity hypoventilation syndrome (OHS), sexual dysfunction, and infectious disease. The essential role of the RD in obesity treatment and optimizing nutrition status in those with these obesity-related comorbid conditions is also described.
The Disease of Obesity
While the consequences of obesity are undisputed, defining obesity itself as either a chronic disease or merely a condition that precedes and causes other systemic diseases is highly debated. In June 2013, the American Medical Association (AMA) declared obesity a disease, reaching a milestone in the effort to improve the lives of those who suffer from obesity.4 However, this statement also aroused passionate debate among health care practitioners, patients, federal institutions, and industries about whether obesity is in itself a bona fide disease or merely a condition that increases risk factors for subsequent disease.
Proponents of the disease classification claim that obesity is a pathophysiological illness that dramatically reduces quality of life, causes or exacerbates weight-related conditions, and shortens the life span.4 Proponents of the obesity disease definition include prominent national and international medical, governmental, scientific, and academic societies such as the WHO, the American Society for Metabolic and Bariatric Surgery, the Obesity Society, and American Association of Clinical Endocrinology.5-8 Many proponents hope that recognizing obesity as a disease will extend advocacy, education, and research toward prevention and treatment to improve the lives of those affected. It’s their hope that greater professional and public awareness will also result in extended insurance coverage for the identification, prevention, and treatment of obesity; influence public policy; and eliminate the social stigma that often surrounds obesity.
However, some members of the medical, scientific, and academic communities oppose the obesity definition, and claim that obesity can’t be defined as a disease because the tool used to diagnose it, BMI, is flawed and doesn’t actually measure body fat accumulation as defined by the WHO. The WHO defines obesity as “abnormal or excessive fat accumulation that may affect health.”2 BMI was designed as a tool to screen obesity risk at the population level and doesn’t indicate the level of fat or body composition of an individual. For example, a person with what is categorized as normal BMI (18.9-24.9) may actually have excessive adipose tissue and display fat-related comorbidities.2 In addition, research shows that not all people who suffer from obesity suffer from other diseases and are “metabolically healthy.”9 Antony D. Karelis, PhD, asserted some obese individuals appear to be metabolically protected from obesity-related complications and conditions. He commented on a study that showed more than one-third of obese individuals had favorable metabolic profiles, eg, normal blood pressure, lipids, insulin sensitivity, and normal inflammatory markers like C-reactive proteins.9
In addition, there’s no universal and authoritative definition of “disease.” Many definitions of “disease” can be found in literature and are typically associated with the system or structure that’s afflicted, such as Crohn’s disease. According to Merriam-Webster’s online medical dictionary, disease is defined as “an impairment of the normal state of the living animal or plant body or one of its parts that interrupts or modifies the performance of the vital functions, is typically manifested by distinguishing signs and symptoms, and is a response to environmental factors (such as malnutrition, industrial hazards, or climate), to specific infective agents (such as worms, bacteria, or viruses), to inherent defects of the organism (such as genetic anomalies), or to combinations of these factors.”10 Opponents argue obesity doesn’t meet the definition and criteria of “disease” in some interpretations, and it remains unclear if the newly recognized classification will improve health outcomes. Even the AMA’s own Council on Scientific Affairs disputed the ruling, requested a review of the evidence, and settled on regarding obesity as a “disorder” or “condition” rather than a medical disease.4
However, despite the often-heated debate over whether obesity is a disease, a condition, or a risk factor, one thing is readily accepted: There is a positive association among increasing BMI, obesity, and weight-related comorbid conditions.5,6,11 In total, more than 60 conditions, such as type 2 diabetes mellitus, hypertension, cardiovascular disease, stroke, gallbladder disease, and even certain cancers, spanning every organ system, are positively associated with obesity.5,11-13
Following a brief overview of the etiology of obesity, this course describes the following conditions: OHS, sexual dysfunction, and infectious disease.
Etiology and Consequences of Obesity
Obesity is recognized as a modern pandemic with concomitant multifactorial and complex causes.11-13 Energy imbalance induced by excessive caloric intake and reduced caloric expenditure from inactivity are recognized as leading causes of obesity.1,2,11,13 Other contributing factors to obesity are less clear but appear to involve genetics, metabolism, culture, environment, psychology, and secondary diseases such as hypothyroidism and Cushing’s syndrome.11-13
Increased technology, urbanization, and changes in food acquisition and preparation have been shown to contribute to obesity. Nutrient-poor, calorie-dense food choices and inconsistent eating patterns also are factors. Research shows reduced intake of healthful foods such as fruits and vegetables along with increased intake of sugar and processed foods, and poor dietary eating patterns such as fad dieting or skipping meals, contribute to obesity.11-15
Obesity is detrimental to the welfare of the individual, society, and the economics of the country.12,16,17 The tangible burden of obesity is expressed as morbidity and mortality and in terms of prevalence and relationship to chronic diseases.9,16,17 Obesity is a major contributing cause of comorbid conditions that affect the physiology of all major organ systems of the human body. Over the course of a lifetime, it increases one’s risk for endocrine dysfunction, cardiovascular diseases, gastrointestinal diseases, pulmonary diseases, musculoskeletal disorders, sexual and reproductive disorders, and certain cancers.11-13,17,18
Coined terms such as “diabesity” denote the widely accepted and prevalent relationship between type 2 diabetes and obesity. Hypertension, osteoarthritis, dyslipidemia, myocardial infarction, and thrombosis are the more commonly reported consequences of obesity.17,18
While the aforementioned comorbidities have been widely researched, dietitians should be aware of lesser-discussed conditions of obesity in order to perform better nutrition-focused physical exams and provide subsequent medical nutrition therapy and obesity treatment/prevention strategies. These include OHS, sexual dysfunction, and infectious disease.
OHS
OHS, also known as Pickwickian Syndrome, is a respiratory disorder characterized by dysfunctional breathing and absence of deep breathing that leads to high levels of carbon dioxide (hypercapnia) and low levels of oxygen (hypoxia) in the blood.19-21 OHS is more prevalent in patients who present with a triad of these conditions: obesity, hypoventilation while awake, and coexisting sleep-disordered breathing (sleep apnea) not caused by medications, neurologic, neuromuscular, or cardiopulmonary explanation for the hypoventilation and carbon dioxide retention.19-21 Research shows there is a higher incidence of OHS in middle-aged males.19
According to Chau and colleagues, OHS is defined as hypercapnia (too much carbon dioxide in the blood) while awake caused by hypoventilation during the daytime, and this is what differentiates OHS from sleep apnea and other chronic obstructive pulmonary disorders.21
Approximately 90% of patients with OHS also present with obstructive sleep apnea (OSA).21 Serious complications of OHS include respiratory acidosis, hypertension, pulmonary hypertension, pulmonary embolism, cor pulomonale (enlargement and failure of the right ventricle of the heart), and subsequent heart failure, as well as compromised quality of life relating to depression, fatigue, sexual dysfunction, headaches, migraines, and daytime sleepiness.21
OHS is positively correlated with BMI.19-21 Not all patients with obesity present with OHS; however, all OHS cases present with BMIs greater than 30 kg/m2. As such, cases of OHS are predicted to increase with the rising obesity epidemic.20,21 The exact cause of OHS is unknown but experts suggest causes of OHS could be rooted (either alone or in tandem) in the following: abnormal leptin levels, labored breathing due to central adiposity, and impaired compensatory response to hypercapnia due to obstructive apneas and sleep apneas.20-25
Leptin, a protein produced by adipose tissue, functions to control appetite and energy expenditure.23-25 The normal response of leptin in proportion to fat storage is to signal the hypothalamus to decrease appetite and food intake and increase metabolism and energy expenditure.23-25 Those with obesity are theorized as having leptin resistance, which is then believed to promote OHS.23-25
Leptin plays a physiologic role beyond metabolism and control of food intake. Leptin is known also to influence the immune system, stimulate proinflammatory cytokines, increase the sympathetic nervous system to control endothelial function, and regulate blood pressure.23-25 Leptin also plays a role in respiratory function by modulating the development of lung tissue and stimulating respiratory control.23-25 Malli and colleagues reviewed evidence that indicates leptin regulates lung tissue growth and maturity and stimulates ventilation. However, in animal models using the mutated ob/ob mice that are obese, it’s believed that leptin-resistance is positively correlated with OHS by increasing the frequency of breathing, minute ventilation, and tidal volume. This, in turn, can elevate arterial pressure of carbon dioxide and depress the hypercapnic ventilator response often seen in OHS.23 It’s unclear, however, whether high serum leptin is a cause or consequence of OHS.23-25
Central adiposity is also believed to play a role in OHS. Central adiposity is defined as an excessive accumulation of abdominal fat often associated with the “apple” body shape. Waist measurements of 40 inches or greater in men and 35 inches or greater in women indicate higher visceral fat and central adiposity.19,20 So far research has shown that those with central adiposity are at increased risk of diabetes, heart disease, and metabolic syndrome.1,2,5,6,11,13
With relation to OHS, central adiposity is believed to hinder the normal breathing mechanism by imposing an excessive load on the organs of the respiratory system and impairing the respiratory muscles and diaphragm, thus increasing the resistance of the upper airway. This in turn causes shallow breathing which then leads to hypoventilation and subsequent hypercapnia.19,21 In addition, central adiposity adversely affects the mobility of the diaphragm leading to reduced lung volumes and contributing further to hypoxemia and hypercapnia, causing respiratory acidosis.19,21 Disruption of appropriate compensatory response to hypercapnia is marked by hypoventilation, impaired respiratory mechanics, and reduced lung volumes.19,21
OHS and the Role of Nutrition and RDs
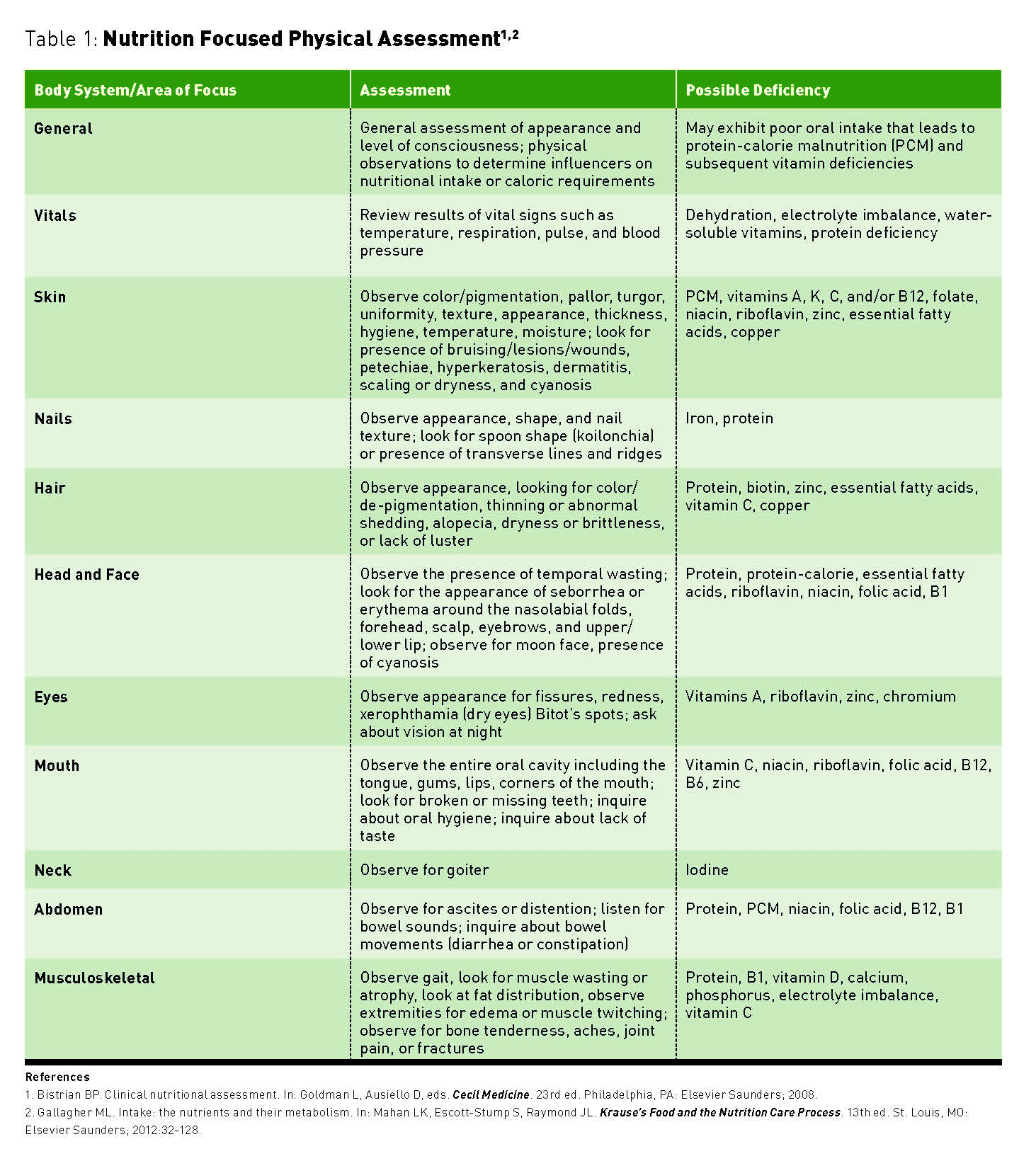
Patients with OHS often present with symptoms of fatigue, morning headaches, choking at night, excessive daytime sleepiness (hypersomnolence), edema of the lower extremities, dyspnea, and loud snoring.19-21 Performing a nutrition-focused physical examination (NFPE) of these patients is appropriate. A NFPE is a system-based assessment of each region of the body. In patients presenting with OHS, the NFPE may reveal cyanosis of the lips, skin, fingers, and toes, and edema of the extremities. See Table 1 for a general summary of a NFPE.
The medical goals in treating patients with OHS include improving gas exchange, lung volume, and central respiratory drive.19-21,25 These goals are accomplished by some or all of the following: using continuous positive airway pressure (C-PAP) and bilevel positive airway pressure (Bi-PAP) machines, medications such as medroxyprogesterone, acetazolamide, and theophylline, and weight loss through either conventional or surgical means.19,21-27
When counseling obese patients with OHS through dietary and behavioral modification, dietitians should provide nutrition guidance specific to this condition, including promoting the restriction of alcoholic beverages, since alcohol depresses the respiratory system.28 In addition, patients should be advised about food-drug interactions. For example, patients prescribed theophylline should restrict caffeine-containing foods such as coffee, tea, cola, and chocolate because caffeine can increase the side effects of theophylline and cause nausea, vomiting, insomnia, irregular heartbeat, and seizures.28
Bariatric surgery, when leading to weight loss, has been shown to improve pulmonary function and gas exchange in patients with OHS.22,26 Marti-Valeri and colleagues showed improvement of hypoxemia, a reduction of hypercapnia, and reduction in the need for C-PAP or Bi-PAP one year after achieving significant weight loss with gastric bypass surgery. The researchers concluded that improvement of arterial blood gases and respiratory function was directly related to the percentage of weight loss at one year after surgery.26 However, bariatric surgery isn’t without nutritional risk, and when undergone by patients, RDs must be sure to provide thorough postsurgical bariatric nutrition guidelines.
Obesity and Sexual and Reproductive Dysfunction
As previously mentioned, metabolic consequences of obesity, notably hypertension, diabetes mellitus, and dyslipidemia, are well documented.1-6,11-13,17 The triad of these conditions is appropriately coined the metabolic syndrome. A direct consequence of metabolic syndrome and obesity is sexual dysfunction in men and women.29
Sexual dysfunction in men manifests as erectile dysfunction (ED) and is defined as the “consistent or recurrent inability to attain and/or maintain penile erection sufficient for sexual activity.”29 Female sexual dysfunction (FSD) is defined as “persistent or recurrent disorders of sexual interest/desire, disorders of the subjective and genital arousal, orgasmic disorders, and pain and difficulty with attempted or incomplete intercourse.”29 In addition to contributing to FSD, obesity increases the risk of reproductive disorders such as polycystic ovary syndrome and infertility, and complications of preconception and pregnancy such as gestational diabetes mellitus (GDM), preeclampsia, and gestational hypertension.29,30
Obesity and Sexual and Reproductive Dysfunction in Males
ED was once thought of as a natural consequence of the aging process. However, results of the Health Professional’s Follow Up Study (HPFS) identified several modifiable health behaviors associated with erectile and sexual function.31 The HPFS, a prospective clinical study sponsored by Harvard’s School of Public Health in collaboration with the National Cancer Institute that began in 1986, is investigating the relationship between nutritionally related factors and diet on diseases such as cardiovascular, cancer, and others within the male population.32 The subjects recruited are employed in the health professions such as osteopathic doctors, pharmacists, veterinarians, dentists, podiatrists, and optometrists.32 One area being studied by the HPFS is the influence obesity and BMI has on disease. The HPFS shows that body leanness and physical activity are strongly associated with reduced risk of ED.31 The HPFS showed that subjects with a BMI greater than 28 kg/m2 had a 30% higher risk for ED.31 Risk factors including increased BMI, physical inactivity, smoking, and alcohol consumption increased prevalence of ED.31 This study also showed that central adiposity, insulin resistance, systemic inflammation and circulation of proinflammatory cytokines, and endothelial dysfunction were all commonly observed in obese men with ED.31
In 2000, Derby and colleagues examined the association between obesity, lifestyle factors, and risk of developing ED in 593 men.33 The researchers showed that men who had a BMI greater than 50 kg/m2 had a higher incidence of ED compared to men with a normal BMI. In another study investigating the relationship between obesity and coronary heart disease risk factors as predictors of ED among 570 subjects, researchers found that a BMI greater than 28 kg/m2 was a significant predictor of ED independent of hypercholesterolemia and age.34
Esposito and colleagues asserted that men with ED were more likely to have greater central adiposity and increased waist measurement, obesity, and concurrently high blood pressure and hypercholesterolemia.35 Corona and colleagues concurred that the most prevalent form of sexual dysfunction in men with metabolic syndrome was ED, with 96% of obese men presenting with this condition.36 In addition, 40% of men with metabolic syndrome expressed suppressed sexual desire and 5% exhibited delayed ejaculation. Compared to healthy, nonobese men, low levels of testosterone and subsequent hypogonadism was observed to be more prevalent in aging, obese men with metabolic syndrome.36
While pharmacological agents such as sildenafil (Viagra) or tadalfil (Cialis) are the standard first-line treatment for most patients with ED, limited studies have shown some naturally occurring nutrients, such as arginine, maca, ginseng, ginkgo biloba, and DHEA, to improve ED in certain cases.37
Arginine is an amino acid found in nuts, legumes, seafood, poultry, eggs, and some vegetables. L-arginine is the precursor of nitric oxide, integral to the proper vascular and endothelial function necessary for erection.37 Ginseng, ginkgo biloba, and maca root have also been shown to influence the function of nitric oxide, whereas DHEA shows limited use as a sexual enhancer.37 While further research is needed to gain insight on the relationship between these nutrients and ED treatment, RDs should be aware of what foods naturally contain these components to better educate their patients and practice prudence when recommending these nutrients in the supplement form.
The RD can influence positive treatment of ED by counseling the patient about weight loss and treatment for metabolic syndrome. In particular, the Dietary Approaches to Stop Hypertension (DASH) diet is clinically shown to reduce hypertension and may indirectly prove useful in the treatment of ED. Using a systematic literature search on the role or effect of diet on ED, Esposito and colleagues showed that diets high in fruits, vegetables, whole grains, nuts, and fish, and low in red meat and processed grains showed more effectiveness in ameliorating ED.38 These types of foods are typically represented in Mediterranean and DASH diets and are believed to improve ED indirectly by having positive effects on blood pressure, reducing inflammation and oxidative stress, and improving cardiac and endothelial function.38 Until any new evidence emerges on how nutrition may improve ED directly, any dietary recommendations specific to patients with ED would do well to stick to the preceding parameters.
Obesity and Sexual and Reproductive Dysfunction in Females
Research investigating the relationship between obesity and FSD is scarce. In an early study by Kirchengast and colleagues (1996), the researchers found a positive relationship among body weight, BMI, and degree of reduced sexual interest.39 The researchers were investigating the relationship among body composition, androgen levels, and sexual interest in 171 postmenopausal women and found those with higher body weight and higher subcutaneous fat in the chest, waist, and hips suffered from sexual disinterest.39 In a more recent study, Esposito and colleagues (2008) showed that obesity negatively affected several aspects characteristic of FSD including arousal, lubrication, and satisfaction.40 Using the Female Sexual Function Index (FSFI), a 19-item, validated self-report questionnaire, the researchers identified a negative relationship among body weight, sexual function, and abnormal FSFI score.40 However, unlike the results from Kirchengast and colleagues, these researchers reported that central fat distribution didn’t correlate with the FSFI score and suggests the total fat amount rather than its distribution affects greater FSD.40 Women with metabolic syndrome also have an increased prevalence of FSD compared to women without metabolic syndrome.41 These results suggest that these patients may also benefit from the DASH diet as an initial treatment for metabolic syndrome.41
More research has been done on the effects of obesity in pregnancy with regard to maternal complications during preconception and pregnancy, as well as postpartum consequences and fetal complications both during development and postnatal. In a multicenter, prospective study, Weiss and colleagues associated an increased risk for GDM, gestational hypertension, preeclampsia, and fetal macrosomia in obese mothers with BMIs of 30 to 39.9 compared with those less than 30.42 Regarding preconception, obesity negatively affects the fertility of women and is linked to neuroendocrine and ovarian dysfunction.42
Early reproductive dysfunction seen with obesity includes precocious menarche (early puberty before the age of 8), irregular menstrual cycles, dysmenorrhea (painful menstrual cycle), amenorrhea (absence of menstrual cycle), and chronic anovulation (absence of ovulation).43 Obesity is also an independent risk factor for miscarriage in women who conceive through in vitro fertilization.44 Obesity and antepartum complications include increased risk for GDM, hypertensive disorder, preeclampsia, thromboembolism, intrauterine fetal death, and stillbirth.45
The exact causes of preeclampsia in obese women isn’t known, but it’s suspected to be caused by increased oxidative stress and altered vascular function caused by infiltration of white blood cells called neutrophils.46 Preeclampsia—diagnosed by the presence of a systolic and diastolic pressure of >140 and >90 mm Hg, respectively, and concomitant 24-hour proteinuria >0.3 g—is a cause of maternal morbidity and mortality. Some estimates show that up to 15% of maternal deaths can be directly attributed to preeclampsia and eclampsia.47
It’s hypothesized that nutrition plays a role in preventing preeclampsia. While it is known that obesity increases the risk of preeclampsia, it’s surmised that calcium, vitamin E, arginine, folate, oleic acid, and carotenoids can play a role in the prevention of preeclampsia, although the exact contributing mechanism is unknown.48
Obese women also have higher incidences of intrapartum complications such as poor labor progress. Sheiner and colleagues found that obesity is an independent risk factor for the need for Cesarean birth.49 In addition, obesity is associated with increased need for labor induction with a significantly greater risk of uterine dehiscence, rupture, morbidity, and injury to the newborn.50 Maternal obesity also affects the gestational weight for age of neonates. Macrosomia, excessive birth weight, has increased and can be attributed to increased insulin resistance and higher plasma triglycerides of the mother that can be transferred to the growing fetus.51 Fetal hyperinsulinemia may also contribute to macrosomia.51 For these women, nutrition counseling to prevent/control GDM is necessary to reduce the risk of these fetal comorbidities. GDM is defined as the presence of diabetes in varying degrees during pregnancy.52 Abnormally high blood glucose, carbohydrate intolerance, and ketonuria, excretion of ketones in the urine, are common symptoms of GDM.52 The strategies of MNT for GDM include emphasizing low-fat, low-sugar, and carbohydrate-controlled food choices with moderate energy restriction, and promoting appropriate weight gain during pregnancy.52,53 Achieving normal glucose levels and preventing excretion of ketones, while meeting the nutritional needs of both mother and fetus, is also a goal and can be best achieved with patient-centered MNT facilitated by an RD.53
Obesity and the Influence on Infectious Disease
The WHO defines an infectious disease as one that can be spread from person to person either indirectly or directly and is caused by microorganisms such as bacteria, viruses, parasites, or fungi.54 Epidemics of infectious diseases have been documented throughout history. From the bubonic plague in the 14th century to the more current HIV, malaria, and influenza that continue to devastate populations in the 21st century, infectious disease hasn’t been obliterated. However, advancements in medicines such as antibiotics and antivirals, and procedures such as the practice of vaccination, universal precautions and sterile environments, have made a significant contribution to saving lives and reducing human suffering. According to the Centers for Disease Control and Prevention, infectious disease causing polio, smallpox, tetanus, diphtheria, measles, mumps, and rubella have nearly been eradicated.55
However, as incidence of infectious disease waned, noninfectious, noncommunicable, chronic disease prevails as the major cause of death and disability on a global scale. Chronic, noninfectious diseases such as obesity, diabetes, heart disease, and others leads to a death toll greater than that seen with infectious diseases including HIV, malaria, and tuberculosis.54,56 According to the WHO, today more than 60% of total deaths worldwide are attributed to chronic disease.56
Paradoxically, while defined as a chronic disease by the AMA and a risk factor for noncommunicable disease by the WHO, obesity is shown to increase the risk of infectious disease.56 As obesity is regarded as inflammatory and immunosuppressive, studies show obese individuals have impaired immune function, leaving them more susceptible to infectious diseases such as tuberculosis, influenza, coxsackie virus, encephalomyocarditis, and helicobacter pylori.57 Obese and hospitalized patients are also at greater risk for nosocomial infections and secondary infections such as sepsis, pneumonia, wound and surgical-site infections, and bacteremia.58
In addition, as previously described, since obesity compromises the pulmonary system, hospitalized obese patients are at higher risk for respiratory infections.59 One explanation for increased susceptibility relates to how obesity negatively affects the immune system by impairing the function and amount of specific cellular players of the immune response.57
Obesity is shown to decrease the overall number of lymphocytes, specifically the macrophages, T-cells, B-cells, and natural killer cells.57,60 In addition to lowering the amount of immune cells, obesity negatively affects the activity of these cells and reduces the body’s ability to respond to pathogenic activity.60 Since obesity is considered systemically inflammatory, there’s increased circulation of tumor necrosis factor (proinflammatory) with concomitant decrease or dysregulation in other immune-mediated cytokines.60
Obesity is considered an independent risk factor for morbidity and mortality from H1N1 influenza. Louie and colleagues noted extreme obesity was associated with increased odds of death from H1N1.61 In a prospective, observational and multicenter study, Diaz and colleagues found patients admitted to the ICU in Spain who were infected with H1N1 and concomitantly obese with a BMI greater than 30, utilized more health care resources because they required longer mechanical ventilation, longer ICU stay, and longer overall hospitalization. In this study, increased mortality was not observed.62
Research also finds obesity to negatively affect the response to vaccinations by decreasing the body’s ability to produce protective antibodies. Sheridan and colleagues showed that high BMIs positively correlated to declining antibody titers after influenza vaccination.63 In addition, obesity decreased the function of CD8+ receptors and memory T-cells, thereby reducing the immune system’s ability to protect the body from progression and rapid severity of the influenza disease.57
Studies have shown reduced efficacy of other vaccines such as the hepatitis B vaccine. Young and colleagues found that a standard three-dose vaccination of hepatitis B had only a 71% protection rate in subjects who had BMIs of 30 or higher compared to 91% in lean subjects.64 Conclusions from these studies imply that response to vaccinations may be suboptimal for obese patients, thereby providing limited protection.
Nutrition and the Immune System
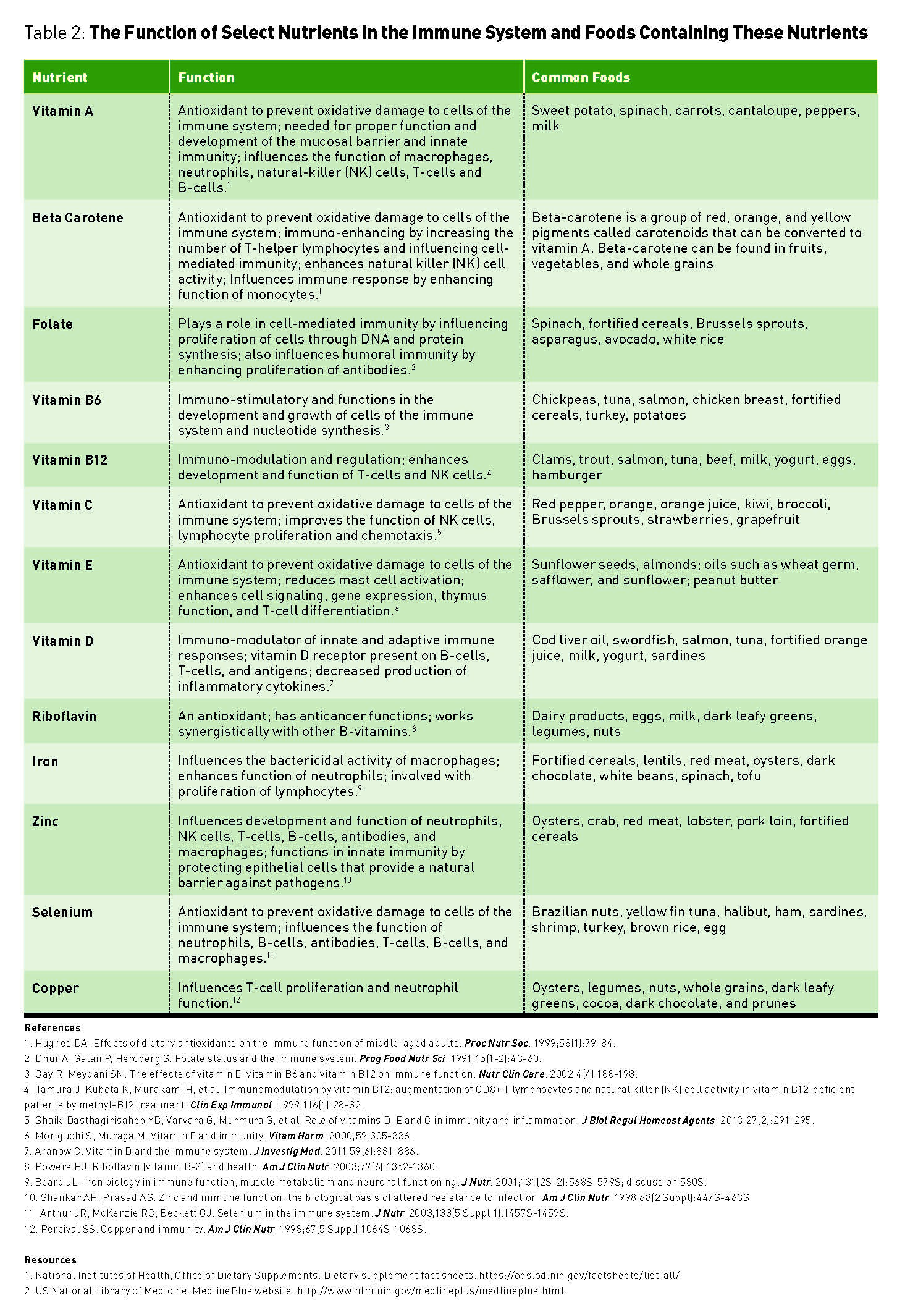
What does this all mean for the nutrition professional? The immune system is highly complex and intricately intertwined with nutrition. See Table 2 for a summary of nutrients, their function in the immune system, and foods that contain that particular nutrient.
Nutrients that affect the immune system function either synergistically or antagonistically, and their availability or deficiency may enhance or impair the immune system.65 For example, a deficiency of both selenium and vitamin E is shown to impair thymus function, deplete lymphocytes, and subsequently suppress humoral immunity responsible for antibody production.65 Vitamin E deficiency is also linked to higher production of prostaglandins, which are immunosuppressive.
Vitamins A and D have a synergistic effect on the maturation and function of monocytes. Vitamins E and C also have a synergistic effect on the reduction of the immunosuppressive arachidonic acid. Zinc deficiency is highly associated with a suppressed immune system by restraining the function of the thymus gland, lymphocyte production, and development and B-cell function.65
This information is relevant to the nutrition professional because obesity itself is a form of malnutrition that presents commonly with vitamin and mineral deficiencies. Research shows obese individuals present with deficiencies in vitamin D, thiamin, folic acid, iron, B12, zinc, phosphorus, B6, and potassium.66
In addition, Kaider-Person and colleagues found that serum levels of vitamins A, E, and C are also significantly lower in obese individuals than in the nonobese population.67 Since more research needs to be done on the effects of individual nutrient supplementation, a dietary recommendation RDs can make is to encourage their clients to follow a balanced diet consisting of nutrient-dense foods. If individual nutrient supplementation is recommended to treat a particular deficiency, dietitians should be aware that the interactions of nutrients with the immune system may have a synergistic or antagonistic effect, and the goal should be to avoid excessive intakes of singular nutrients. Laboratory studies to monitor vitamins and minerals should be incorporated as a part of an interdisciplinary and patient-centered approach to care.
Current Treatment Modalities for Obesity
While this article addresses the less-discussed conditions caused by obesity and their treatment, treating obesity involves prevention, which is the goal of many local and federal initiatives. However, for those who already suffer from this disease and related consequences, a variety of successful treatment options exist. It’s broadly recognized that a weight loss of 5% to 15% significantly reduces health-related risks of obesity.68,69 Recognized treatment modalities include individualized, interdisciplinary programs that promote lifestyle changes through regimens tailored to address the psychosocial, dietary, and physical activity requirements for weight loss.68,69
Pharmacotherapy and antiobesity drugs have been developed and are intended to be used in conjunction with these traditional obesity treatment programs. According to the National Institutes of Health’s 57-NHLBI Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults, weight loss drugs can be useful in patients with BMIs greater than 30 with no concomitant risk factors in conjunction with weight loss programs and continued monitoring by a physician for efficacy and safety.69
Weight loss medications haven’t been shown to be without risks. In the early 1970s, fenfluramine was introduced as an appetite suppressant and weight loss medication. However, in 1997, fenfluramine (Fen-Phen, brand names: Adipex-P, Fastin, et al) was taken off the market because of pulmonary and cardiovascular safety concerns. In 1997, sibutramine (brand name: Meridia) was subsequently approved by the FDA but removed from the market in 2010 as a result of concerns about cardiovascular safety.70
Currently used antiobesity medications are: orlistat (over-the-counter name: Alli; prescription strength: Xenical), lorcaserin (brand name Belviq), and phentermine/topiramate combination (brand name: Qsymia). While lorcaserin and phentermine/topiramate are the first two new antiobesity medications approved in more than 13 years, and double-blind clinical trials on both showed positive results in efficacy and safety, the FDA is requiring long-term postmarketing studies to include outcomes trials on cardiovascular risk.71
Metabolic and bariatric surgery is recognized as a long-term treatment option for obesity.72 Historically, there have been many surgical variations of bariatric surgery including the jejunoileal bypass and the vertical banded gastroplasty. However, these procedures are no longer performed, partly because of high complication rates and the advent of newer, safer procedures. The four major bariatric procedures performed worldwide are biliopancreatic diversion with/without duodenal switch, the adjustable gastric band, the Roux-en-Y gastric bypass, and the sleeve gastrectomy, with the latter becoming the fastest-growing bariatric procedure worldwide because of successful patient outcomes and fewer complications.72 (“Vertical Sleeve Gastrectomy — Considerations and Nutritional Implications,” a course by this author, is available at www.todaysdietitian.com/pdf/courses/CraggsDinoVSG.pdf.)
The total number of bariatric surgeries performed worldwide from 2008 to 2011 exceeded 340,000.72 In 2011, the United States and Canada performed more than 101,000 bariatric surgeries and more than 19% were sleeve gastrectomy.72 Reductions in BMI at one year for the gastric bypass, sleeve gastrectomy, and adjustable gastric band were 15.34, 11.87, and 7.05, respectively, indicating positive weight loss outcomes.73 In addition to positive weight loss, the popularity of bariatric surgery comes from effective amelioration of comorbid conditions such as type 2 diabetes, hypertension, and OSA.73 Hutter and colleagues reported that patients who underwent gastric bypass experienced an 83%, 79%, and 66% remission of type 2 diabetes, hypertension, and hyperlipidemia and OSA, respectively.73
In the Surgical Therapy and Medications Potentially Eradicate Diabetes Efficiently (STAMPEDE) Trial, a recent single-center, three-arm, randomized, controlled study, 150 patients were randomized into one of three intervention groups. Group 1 received no bariatric surgery but received MNT to treat diabetes according to the guidelines of the American Diabetes Association. This intervention included lifestyle counseling, weight management, home glucose monitoring, and pharmacotherapy using the incretins.74
Groups 2 and 3, respectively, received MNT and bariatric surgery, the sleeve gastrectomy, or the gastric bypass. Eligibility criteria included patients with uncontrolled type 2 diabetes of more than eight years, an A1c greater than 7%, (mean A1c was 8.9% to 9.5%) and metabolic syndrome (high lipids, high Bp); between the ages of 20 and 60 with a BMI from 27 to 43. All patients were treated with glucose-, lipid-, and blood pressure-lowering medications.74
Results showed that rapid improvement was seen in the first three months with surgery compared with a more gradual improvement with medical therapy. Interestingly, the surgical group showed more positive outcomes in terms of medication usage. The average number of diabetes medications per patient per day increased in the medical therapy group, but significantly decreased in the surgical groups. Insulin remained high at 38% in the medical therapy group, but was reduced to 4% and 8% in the gastric bypass and sleeve gastrectomy groups, respectively. In addition, there was an increase in HDL and a reduction in total cholesterol after the surgeries compared to that achieved through medical therapy.74
Conclusion
While there’s disagreement about whether obesity is a disease or condition, it’s universally accepted that obesity causes conditions that can lower quality of life and endanger the overall health and well-being of the individual. This article highlights the lesser-mentioned disorders of obesity to bring to the forefront the magnitude and far-reaching negative health effects.
The role of RDs is to work collaboratively across programs and in an interdisciplinary approach with other health care professionals. While it’s ideal to prevent obesity in the first place, nutrition professionals can assess the individual needs of patients with existing obesity and make dietary recommendations based on their specific needs and comorbid influences. Obesity itself is complicated to treat. However, with the help of RDs, there’s hope for patients who suffer from obesity and its consequences. RDs can affect and positively influence patients’ well-being through appropriate and patient-centered nutrition recommendations.
— Written by Lillian Craggs-Dino, DHA, RDN, LDN, a national and international speaker, a freelance food and nutrition writer in South Florida, and a practicing bariatric dietitian and support group coordinator for a renowned bariatric program in South Florida.
References
1. Centers for Disease Control and Prevention. Adult obesity facts. http://www.cdc.gov/obesity/data/adult.html. Updated June 16, 2015.
2. World Health Organization. Obesity and overweight. http://www.who.int/mediacentre/factsheets/fs311/en/. Updated January 2015.
3. GBD 2013 Mortality and Causes of Death Collaborators. Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2015;385(9963):117-171.
4. American Medical Association. Report 4 of the Council on Scientific Affairs A-105). http://www.ama-assn.org//meetings/public/annual05/csa4a05.pdf
5. James WPT. WHO recognition of the global obesity epidemic. Int J Obes (London). 2008;32 (Suppl 7):S120-S126.
6. Disease of obesity. ASMBS website. http://asmbs.org/patients/disease-of-obesity
7. TOS applauds the American Medical Association for recognizing obesity as a disease. Obesity Society website. http://www.obesity.org/news-center/tos-applauds-ama-for-recognizing-obesity-as-a-disease.htm
8. Obesity is a disease: The American Medical Association agrees with the American Association of Clinical Endocrinologists. American Association of Clinical Endocrinologists website. http://media.aace.com/press-release/obesity-disease-american-medical-association-agrees-american-association-clinical-endo
9. Karelis AD. Metabolically healthy but obese individuals. Lancet. (2008):372(9646);1281-1283.
10. Disease. Merriam-Webster Medical Dictionary website. http://www.merriam-webster.com/medical/disease
11. O’Brien PE, Dixon JB. The extent of the problem of obesity. Am J Surg. 2002;184(6B):4S-8S.
12. Rosin O. The economic causes of obesity: a survey. J Econ Surv. 2008;22(4):617-647.
13. Pi-Sunyer FX. The obesity epidemic: Pathophysiology and consequences of obesity. Obes Res. 2002;10 (Suppl 2):97S-104S.
14. O’Neil CE, Nicklas TA, Liu Y, Franklin FA. Impact of dairy and sweetened beverage consumption on diet and weight of a multiethnic population of Head Start mothers. J Am Diet Assoc. 2009;109(5):874-882.
15. Ueland O, Cardello AV, Merrill EP, Lesher LL. Effects of portion size information on food intake. J Am Diet Assoc. 2009;109(1):124-127.
16. U.S obesity trends. Centers for Disease Control and Prevention website. http://www.cdc.gov/obesity/data/trends.html#State
17. Calza S, Decarli A, Ferraroni M. Obesity and prevalence of chronic diseases in the 1999-2000 Italian National Health Survey. BMC Public Health. 2008;8:140-149.
18. Fried M, Hainer V, Basdevant A, et al. Interdisciplinary European guidelines on surgery of severe obesity. Obes Facts. 2008;1(1):52-59.
19. Mokhlesi B. Obesity hypoventilation syndrome: a state-of-the-art review. Respir Care. 2010;55(10):1347-1362.
20. Wen E, Aysola R. Obesity hypoventilation syndrome: are you missing the diagnosis? Proc UCLA Healthcare. 2012;16.
21. Chau EH, Lam D, Wong J, Mokhlesi B, Chung F. Obesity hypoventilation syndrome: a review of epidemiology, pathophysiology and perioperative considerations. Anesthesiology. 2012;117(1):188-205.
22. Beckman LM, Beckman TR, Earthman CP. Changes in gastrointestinal hormones and leptin after Roux-en-Y gastric bypass procedure: a review. J Am Diet Assoc. 2010;110(4):571-584.
23. Malli F, Papaioannou AI, Gourgoulianis KI, Daniil Z. The role of leptin in the respiratory system: an overview. Respir Res. 2010;11:152-168.
24. Phipps PR, Starritt E, Caterson I, Grunstein RR. Association of serum leptin with hypoventilation in human obesity. Thorax. 2002;57(1):75-76.
25. Campo A, Frühbeck G, Zulueta JJ, et al. Hyperleptinaemia, respiratory drive and hypercapnic response in obese patients. Eur Respir J. 2007;30(2):223-331.
26. Martí-Valeri C, Sabaté A, Masdevall C, Dalmau A. Improvement of associated respiratory problems in morbidly obese patients after open Roux-en-Y gastric bypass. Obes Surg. 2007;17(8):1102-1110.
27. Piper AJ, Grunstein RR. Obesity hypoventilation syndrome: mechanisms and management. Am J Respir Crit Care Med. 2011;183(3):292-298.
28. Avoid food-drug interactions: a guide from the national consumers league and the US Food and Drug Administration. US Food and Drug Administration website. www.fda.gov/downloads/Drugs/ResourcesForYou/Consumers/BuyingUsingMedicineSafely/EnsuringSafeUseofMedicine/GeneralUseofMedicine/UCM229033.pdf
29. Larsen SH, Wagner G, Heitmann BL. Sexual function and obesity. Int J Obes (Lond). 2007;31(8):1189-1198.
30. Pasquali R, Patton L, Gambineri A. Obesity and infertility. Curr Opin Endocrinol Diabetes Obes. (2007);14(6):482-487.
31. Bacon CG, Mittleman MA, Kawachi I, Giovannuci E, Glasser DB, Rimm EB. Sexual function in men older than 50 years of age: results from the health professionals follow-up study. Ann Int Med. 2003;139(3):161-168.
32. Health Professionals Follow-Up Study. Harvard TH Chan School of Public Health website. http://www.hsph.harvard.edu/hpfs/hpfs_about.htm
33. Derby CA, Mohr BA, Goldstein I, Feldman HA, Johannes CB, McKinlay JB. Modifiable risk factors and erectile dysfunction: can lifestyle changes modify risk? Urology. 2000;56(2):302-306.
34. Feldman HA, Johannes CB, Derby CA, et al. Erectile dysfunction and coronary risk factors: prospective results from the Massachusetts male aging study. Prev Med. 2000;30(4):328-338.
Erectile Dysfunction and Coronary Risk Factors: Prospective Results from the Massachusetts Male Aging Study moreless272727 35. Esposito K, Giugliano F, De Sio M, et al. Dietary factors in erectile dysfunction. Int J Impot Res. 2006;18(4):370-374.
36. Corona G, Mannucci E, Forti G, Maggi M. Hypogonadism, ED, metabolic syndrome, and obesity: a pathological link supporting cardiovascular diseases. Int J Androl. 2009;32(6):587-598.
37. MacKay D. Nutrients and botanicals for erectile dysfunction: examining the evidence. Altern Med Rev. 2004;9(1):4-16.
38. Esposito K, Giugliano F, Maiorino MI, Giugliano D. Dietary factors, Mediterranean diet, and erectile dysfunction. J Sex Med. 2010;7(7):2338-2345.
39. Kirchengast S, Hartmann B, Gruber D, Huber J. Decreased sexual interest and its relationship to body build in postmenopausal women. Maturitas. 1996;23(1):63-71.
40. Esposito K, Giugliano F, Ciotola M, De Sio M, D’Armiento M, Giugliano D. Obesity and sexual dysfunction, male and female. Int J Impot Res. 2008;20(4):358-365.
41. Esposito K, Ciotola M, Marfella R, Di Tommaso D, Cobellis L, Giugliano D. The metabolic syndrome: a cause of sexual dysfunction in women. Int J Impot Res. 2005;17(3):224-226.
42. Weiss JL, Malone FD, Emig D, et al. Obesity, obstetric complications and caesarean delivery rate — a population-based screening study. Am J Obstet Gynecol. 2004;190(4):1091-1097.
43. Arendas K, Qiu Q, Gruslin A. Obesity in pregnancy: pre-conceptional to postpartum consequences. J Obstet Gynaecol Can. 2008;30(6):477-488.
44. Lashen AM, Pasker-de Jong PC, de Boer EJ, et al. Effects of subfertility cause, smoking, and body weight on the success rate of IVF. Human Reprod. 2005;20(7):1867-1875.
45. Doherty DA, Magann EF, Francis J, Morrison JC, Newnham JP. Pre-pregnancy body mass index and pregnancy outcomes. Int J Gynaecol Obstet. 2006;95(3):242-247.
46. Walsh, SW. Obesity: a risk factor for preeclamsia. Trends Endocrinol Metab. 2007;18(10):365-370.
47. Uzan J, Carbonnel M, Piconne O, Asmar R, Ayoubi JM. Pre-eclamsia: pathophysiology, diagnosis, and management. Vasc Health Risk Manag. 2011;7:467-474.
48. Roberts JM, Balk JL, Bodnar LM, Belizán JM, Bergel E, Martinez A. Nutrient involvement in preeclamsia. J Nutr. 2003;133(5 Suppl 2):1684S-1692S.
49. Sheiner E, Levy A, Menes TS, Silverberg D, Katz M, Mazor M. Maternal obesity as an independent risk factor for caesarean delivery. Paediatr Perinat Epidemiol. 2004;18(3):196-201.
50. Hibbard JU, Gilbert S, Landon MB, et al. Trial of labor or repeat cesarean delivery in women with morbid obesity and previous cesarean delivery. Obstet Gynecol. 2006;108(1):125-133.
51. Ehrenberg HM, Iams JD, Goldenberg RL, et al. Maternal obesity, uterine activity, and the risk of spontaneous preterm birth. Obstet Gynecol. 2009;113(1):48-52.
52. Thomas-Doberson D. Nutritional management of gestational diabetes and nutritional management of women with a history of gestational diabetes: two different therapies or the same? Clin Diabetes. 1999;17(4):170-176.
53. Gunderson EP. Gestational diabetes and nutritional recommendations. Curr Diab Rep. 2004;4(5):377-386.
54. Infectious diseases. World Health Organization website. http://www.who.int/topics/infectious_diseases/en/
55. Centers for Disease Control and Prevention. Achievements in public health, 1900-1999: control of infectious diseases. MMWR. 1999;48(29):621-629.
56. World Health Organization. Total NCD Deaths — data by county. http://apps.who.int/gho/data/node.main.A860?lang=enreference
57. Karlsson EA, Beck MA. The burden of obesity on infectious disease. Exp Biol Med (Maywood). 2010;235(12):1412-1424.
58. Cantürk Z, Cantürk NZ, Çetinarslan B, Utkan NZ, Tarkun I. Nosocomial infections and obesity in surgical patients. Obes Res. 2003;11(6):769-775.
59. Kwong JC, Campitelli MA, Rosella LC. Obesity and respiratory hospitalizations during influenza seasons in Ontario, Canada: a cohort study. Clin Infect Dis. 2011;53(5):413-421.
60. Cottam DR, Matter SG, Barinas-Mitchell E, et al. The chronic inflammatory hypothesis for the morbidity associated with morbid obesity: implications and effects of weight loss. Obes Surg. 2004;14(5):589-600.
61. Louie JK, Acosta M, Samuel MC, et al. A novel risk factor for a novel virus: obesity and 2009 pandemic influenza A (H1N1). Clin Infect Dis. 2011;52(3):301-312.
62. Diaz E, Rodriguez A, Martin-Loeches I, et al. H1N1 Semicycu Working Group. Impact of obesity in patients infected with 2009 influenza A (H1N1). Chest. 2011;139(2):382-386.
63. Sheridan PA, Paich HA, Handy J, et al. Obesity is associated with impaired immune response to influenza vaccination in humans. Int J Obes (Lond). 2012;36(8):1072-1077.
64. Young MD, Gooch WM 3rd, Zuckerman AJ, DU W, Dickson B, Maddrey WC. Comparison of triple antigen and a single antigen recombinant vaccine for adult hepatitis B vaccination, J Med Virol. 2001;64(3):290-298.
65. Kubena KS, McMurray DN. Nutrition and the immune system: a review of nutrient-nutrient interactions. J Am Diet Assoc. 1996;96(11):1156-1164.
66. Mechanick JI, Kushner RF, Sugerman HJ, et al. American Association of Clinical Endocrinologists. The Obesity Society, and American Society for Metabolic & Bariatric Surgery Medical Guidelines for Clinical Practice for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric surgery patient. Surg Obes Rel Dis. 2008;(5 Suppl):S109-S184.
67. Kaider-Person O, Person B, Szomstein S, Rosenthal RJ. Nutritional deficiencies in morbidly obese patients: a new form of malnutrition? Part B: minerals. Obes Surg. 2008;18(8):1028-1034.
68. Anderson JW, Konz EC. Obesity and disease management: effects of weight loss on comorbid conditions. Obes Res. 2001;9(4):326S-334S.
69. The practical guide: identification, evaluation, and treatment of overweight and obesity in adults. National Heart, Lung, and Blood Institute website. http://www.nhlbi.nih.gov/files/docs/guidelines/prctgd_c.pdf
70.FDA announces withdrawal of fenfluramine and dexfenfluramine (fen-phen). US Food and Drug Administration website. http://www.fda.gov/Drugs/DrugSafety/PostmarketDrugSafetyInformationforPatientsandProviders/ucm179871.htm. September 15, 1997.
71. US Department of Health and Human Services. Prescription Medications for the Treatment of Obesity. http://www.sumnerdietrx.com/files/2013/03/Prescription_Medications.pdf
72. Buchwald H, Oien DM. Metabolic/bariatric surgery worldwide 2011. Obes Surg. 2013;23(4):427-436.
73. Hutter MM, Schirmer BD, Jones DB, et al. First report from the American College of Surgeons Bariatric Surgery Center Network: laparoscopic sleeve gastrectomy has morbidity and effectiveness positioned between the band and the bypass. Ann Surg. 2011;254(3):410-422.
74. Kashyap SR, Bhatt DL, Schauer PR, STAMPEDE Investigators. Bariatric surgery vs. advanced practice medical management in the treatment of type 2 diabetes mellitus: rationale and design of the Surgical Therapy And Medications Potentially Eradicate Diabetes Efficiently trial (STAMPEDE). Diabetes Obes Metab. 2010;12(5):452-454.